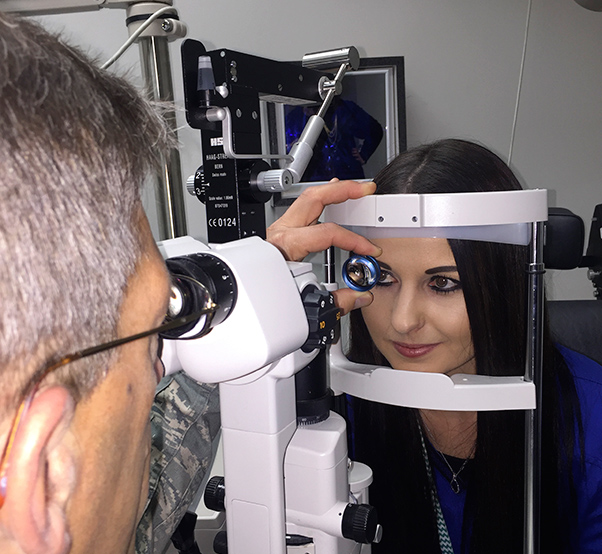
The 412th Medical Group Optometry Team.
The Air Force recognizes the achievements of the men and women who comprise the Biomedical Sciences Corps by designating Jan. 25-29 as BSC Appreciation Week.
The BSC’s roots date back to 1917, when the Sanitary Corps was established to combat infectious diseases, and the Army Medical Administrative Corps followed three years later.
In 1949, the Air Force Medical Service was officially established. The Air Force Medical Service continued to expand over the next two decades and in 1965, the Biomedical Sciences Corps was born.
Over the past 51 years, the BSC continued to expand its range of personnel to include a wide variety of medically-trained professionals.
To date, the BSC’s mission is to enhance Air Force combat capability and effectiveness by providing world-class customer service and scientific expertise, resulting in peak force performance, productivity, and quality healthcare to our beneficiary population.
Comprised of 15 primary specialty codes, the BSC is the most diverse corps in the Air Force Medical Service. Capitalizing on their breadth of expertise, the BSC motto is: United in the Mission.
With 2,400 officers, supported by 5,800 enlisted members in parallel career fields, BSC members can be found at 81 locations around the world and also in multiple settings.
The BSC encompasses physical therapy, optometry, podiatry, physician assistants, audiology, speech pathology, clinical psychology, clinical social work, occupational therapy, aerospace and operational physiology, dietetics, bioenvironmental engineers, public health, medical entomology, pharmacy, biomedical laboratory, healthcare facilities architects/engineers, and health and medical physics.
In addition to specialty roles within our medical treatment facilities, BSC officers are embedded within operational units, serve at every level of medical command, and lead on staffs of the major commands, Forward Operating Agencies, and Headquarters Air Force.
Additionally, the Biomedical Sciences Corps is heavily invested in research and a host of other vital roles to meet the demands of the Air Force mission.
Please join me in recognizing the contributions of the Edwards BSC teams, who dedicate their lives to improving health, maximizing performance, and providing trusted medical care to support our most vital resource, our Airmen and their families. Below is info on all the BSC services here on base.
Bioenvironmental Engineering Team.
Aerospace, operational physiology
The mission involves Human Performance optimization throughout the wing. When we think of weapons systems, people often think of aircraft, bombs/bullets, computer software that interfaces with hardware, etc. We study the most variable of all systems: the human system. What makes human beings better at what they do and what factors can negatively impact their performance as well?
Here at Edwards, the aerospace physiologist officer is a flight commander within the 412th Operations Group supported by an enlisted technician, which is typical at a base of this size and scope. In the future, we hope to grow our team since Edwards has so many unique opportunities to study human performance.
We take ear impressions in order to make custom-fit hearing protection devices for our aircrew, which enhances their ability to communicate with each other in flight. We also teach airsickness management training in our spinning “barany chair” that helps one’s inner ear adapt to three-dimensional rotations. In time, we will become more involved with wing safety and serve as Human Factors consultants for flight and ground incidents and mishaps. We teach classes for all types of aircrew on topics like hypoxia, hyperventilation, stress, fatigue, team dynamics, communication, spatial disorientation and situational awareness all in an effort to enhance their ability to cognitively process information and safely execute their mission in a dynamic flight environment. After a mishap occurs, we are often called to serve as the Human Factors representative on the Safety Investigation Board or the Accident Investigation Board. Since we are considered “regional” trainers, we also teach classes at March Air Reserve Base, California, when requested and we support the night vision lab at NASA. In the future we hope to develop an agreement with NASA that would allow us to utilize their Reduced Oxygen Breathing Device to train our aircrew here so they are not required to go TDY to get the training.
To become an Aerospace Physiology Officer (43A), there is no set degree requirement. However, science degrees in fields like biology, biomedical engineering, exercise physiology, human systems integration, kinesiology are preferred. We are required to obtain continuing education units each year.
The Physical Therapy Clinic at Edwards Air Force Base.
Bioenvironmental engineering team
The Bioenvironmental Engineering team’s core mission is to advise commanders at all levels on health threats and necessary controls to ensure illnesses are prevented before they occur. In a nutshell, we are health risk assessors focused on anticipating, recognizing, evaluating, and controlling health hazards associated with the Air Force activities.
The Edwards BEE team has 28 authorized positions (five officers, 21 enlisted, and two civilian). In addition, the Air Force Research Lab detachment has a civilian and enlisted member supporting their research activities. BEE officers require, at minimum, a bachelor’s degree in an accredited engineering field or certain physical science specialties. Enlisted members complete rigorous specialty training at the USAF School of Aerospace Medicine immediately after graduating from Basic Military Training. Our civilian members must have prior experience in the BEE career field, or comparable educational/experience in the civilian Occupational and Environmental Health sector.
Our team supports a broad range of surveillance activities at Edwards, the Air Force Research Lab site and Plant 42 in Palmdale. General program areas include Occupational Health, Environmental Health, Radiation Health, and Contingency Response.
Aside from day-to-day program responsibilities, BEE has a significant role in the installation disaster response mission. BEE is a member of the emergency response force for a wide range of incidents and accidents, including natural disasters, aircraft accidents, hazardous material spills, and terrorist/CBRN events.
Mental Health Flight, 412th Medical Group.
Mental health team
The Mental Health Flight stands ready to support the Edwards Air Force Base’s mission by strengthening the resiliency and well-being of all service members and their families assigned to the installation.
Our team is composed of three psychologists, three clinical social workers, a psychiatrist, and nine technicians. All of our providers have achieved a doctorate or master’s level degree and their respective licensure. Two of our technicians have master’s degrees and another recently completed her PhD.
The flight is divided into three primary elements: Outpatient Mental Health; Alcohol and Drug Abuse Prevention and Treatment (ADAPT), and the Family Advocacy Program (FAP). In addition, we lead the installation’s Disaster Mental Health Response Team, and Suicide Prevention Program. Our services include: outpatient counseling and psychiatric services, New Parents’ Support Program, 24 hour Command and First Sergeant mental health support and consultation, special duty evaluations, community outreach and resiliency training, PCS and deployment clearances, and Automated Neuropsychological Assessment Metrics testing.
The Mental Health team is growing with the recent additions of a new psychologist and 2 new social workers. We will be extending our outpatient counseling services to our dependent beneficiaries in March 2016. The suicide prevention program leads the AFMC with the highest completion rate of both the annual suicide prevention and frontline supervisor trainings. Our aggressive responsible alcohol use campaign has resulted in a 67% decrease in DUIs, and the fewest DUIs in Air Force Materiel Command for 2015. Family Advocacy has trail blazed new partnerships with community resources resulting in Antelope Valley Hospital achieving its first “baby friendly” facility certification, and inclusion on its sexual assault prevention services board.
The pharmacy at Edwards AFB.
Optometry team
The 412th Medical Group Optometry team’s primary function is to provide vision care for active duty, retirees, and dependents.
Providing vision care on Edwards AFB is a very demanding mission with many benefits. Whether the mission requires a pilot to start wearing corrective glasses to fly a crucial test sortie or ensuring that our security forces members have the optimal vision for bearing arms and defending our base; optometry is always at the forefront, ensuring that the 412th Test Wing achieves mission success.
Our team is qualified to provide care for patients who are 70 years old with longstanding diabetes to a six-month old infant who cannot focus on their mother’s face. We also perform refractive surgery consults and post-operative care, occupational laser eye exams, treat dry eye disorders, diagnose and treat computer vision syndrome and provide vision training for pilots, security forces members, and athletes who are looking for a competitive advantage.
To become an Air Force optometrist, candidates must obtain a bachelor’s degree, followed by an optometry degree, earned after four years of graduate studies. After obtaining an optometry degree, officers must complete three different phases of National Optometry Board examinations before they are qualified to provide care. The amount of continuing education required varies based on the state of licensure, but most states require 20-25 credits per year.
The Physical Therapy clinic at Edwards Air Force Base.
Pharmacy team
The pharmacy at Edwards AFB is composed of eight team members. There are two officers, two enlisted pharmacy specialists and four civilians; or two pharmacists and six technicians. Our purpose is to provide safe and effective medications to our population and to assist our clinical staff with appropriate drug therapy. In doing so, our beneficiaries can maintain their health, prepare for deployment with the necessary medications, or recover from an illness as fast as possible in order to return to duty and ultimately accomplish their mission.
The Medical Group pharmacy fills over 79,000 prescriptions every year. From the time you request your prescription to the time that you walk away with it, it has gone through at least five different processes to ensure it’s safe, appropriate, and accurate. For example, every prescription must go through a rigorous screening process that checks for drug interactions or possible duplications with other medications that you are taking. If potential problems are discovered, the pharmacy will take steps to get you a suitable alternative or counsel you on the potential effects.
Pharmacists go through an extensive training program to obtain a Doctor of Pharmacy degree. Once accepted into pharmacy school, students must complete three years of core classes followed by an additional year of active internship, where students apply their clinical knowledge. Civilian pharmacy technicians accomplish eight months of training to receive their national certification and military pharmacy technicians spend three months in technical school learning medication names, their intended use, how to reconstitute and prepare medications, and how to document patient information in the electronic health record system.
The Physical Therapy clinic at Edwards Air Force Base.
Physician assistants
There are two physician assistants assigned to the 412th Medical Group, Capt. Rochelle Zangen and 1st Lt. Valerie Villanueva.
Combined, these hard-working professionals and their supporting nurses and technicians care for an astounding 2,200 patients assigned to their respective teams and are responsible for nearly 10,000 medical appointments annually. Although assigned to a preceptor physician, Air Force PAs exercise autonomy in medical decision-making and provide a broad range of diagnostic and therapeutic services. Air Force PAs provide a clinical role primarily in family practice, but are given the opportunity to compete for fellowships in other areas, such as orthopedics and emergency medicine. PAs also deploy to provide medical expertise in wartime and humanitarian missions, and play an active role in research and leadership activities.
To become a physician assistant, applicants are required to have a bachelor’s degree and have between 1,000 and 3,000 hours of exposure in clinical care settings. A typical physician assistant program is two years, four months in length, which encompasses a full year of clinical rotations in emergency care, family medicine, general surgery, pediatrics, and women’s health.
412th Medical Group physician assistants.
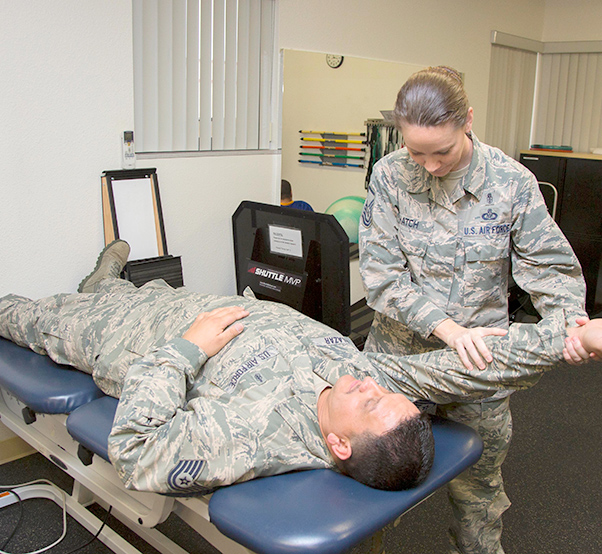
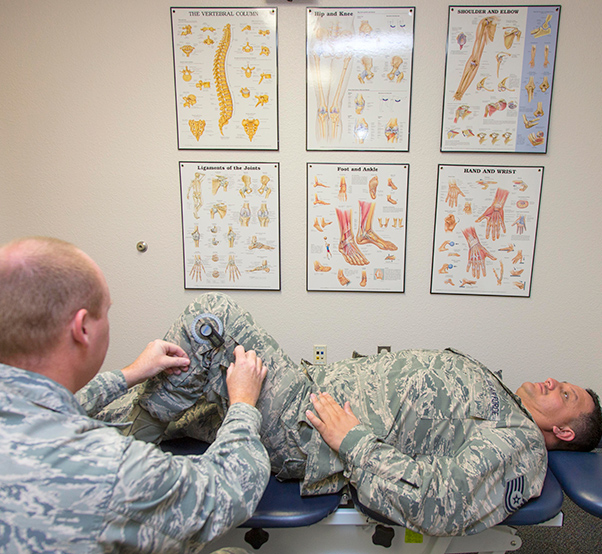
Physical therapy team
The Physical Therapy clinic at Edwards Air Force Base is responsible for the diagnosis and treatment of musculoskeletal injuries and is open to all active duty, dependents and eligible retirees.
Maj. William Clarkson, the Physical Therapy flight commander, completed his Master of Physical Therapy in 2001 at the University of Texas Health Science Center and followed up with his Doctor of Physical Therapy in 2013 from the Texas Tech University Health Science Center. Clarkson is also a Board Certified Clinical Specialist in Orthopedic Physical Therapy with a special interest in the treatment and prevention of running injuries. As a physical therapist, Clarkson is a subject matter aspect on musculoskeletal injuries. He is credentialed to perform a thorough evaluation, order diagnostic imaging, prescribe certain medications, and refer to other specialists. Treatment strategies are comprised of the use of therapeutic exercise and manual therapy techniques including joint manipulation.
The clinic is also staffed with two enlisted Physical Medicine specialists. Master Sgt. Kimberly Hatch is the clinic’s flight chief and Staff Sgt. Jessica Aranda serves as the clinic’s NCOIC. Each specialist completes a 12-week program at the Medical Education and Training Center at Fort Sam Houston in San Antonio, Texas. At the conclusion of this intense training program, the specialists receive their Associates Degree in Physical Therapy and are eligible to take the licensure exam to become a licensed physical therapy assistant. The chief duty of a physical medicine specialist involves progressing their patients through the therapist’s established plan of care. This includes instructing the patient in proper exercise techniques, performing musculoskeletal joint mobilization and soft tissue massage, and the application of neuromuscular electrical stimulators.
The physical therapy clinic at Edwards AFB is one of only a few in the Air Force that allows for active duty patients to be treated without a referral from a physician. This “direct access” program reduces injury-related pain and speeds the recovery process by allowing eligible members to schedule an appointment directly with the physical therapist, drastically cutting down the time from injury to initial treatment.
Biomedical Sciences Corps officers from the 412th Medical Group.
Public health team
The Edwards AFB Public Health Flight consists of one officer, 10 enlisted technicians, and two civilians.
The flight is composed of three elements: Force Health Management, Community Health, and Health Promotions.
The Force Health Management element is the most recognized element and is comprised of the Deployment Health Program, Occupational Health Program, and the Preventive Health Assessment Cell. The Community Health element most closely resembles our civilian counterparts, such as county public health departments, and is comprised of the Communicable Disease Program, Medical Entomology, and Food Safety and Sanitation Program. The newest element to the Edwards PH Flight is the Health Promotions element, which was formerly the Health and Wellness Center, but through an Air Force transformation and realignment now falls under PH. The element is still responsible for all programs that the Health and Wellness Center formerly offered.
To qualify as a Public Health officer, officers must have a Doctorate of Veterinary Medicine, Master of Science in Epidemiology, or a Master of Public Health degree. After the completion of Commissioned Officer Training, all new PHOs attend a ten-week basic Public Health Officer course. In this course, officers learn about the PH mission to prevent, reduce, and control the incidence of communicable diseases amongst Air Force personnel at home and abroad and how to apply preventive/PH techniques to reduce and control the incidence of communicable disease and occupational illnesses.
To become a Public Health specialist, a member must have a high school diploma or GED with fifteen college credits to qualify for a 10-week technical school. Once assigned to a base-level PH team, specialists complete a variety of tasks to include: interviewing and educating patients while ensuring proper treatment for diseases, inspecting food service and public facilities for sanitation standards, and inspecting food to ensure quality and wholesomeness. Specialists also play a key role in ensuring members are cleared and medically able to deploy by overseeing physical exam requirements and occupational health education for workers exposed to physical, biological, and chemical hazards in their workplaces.