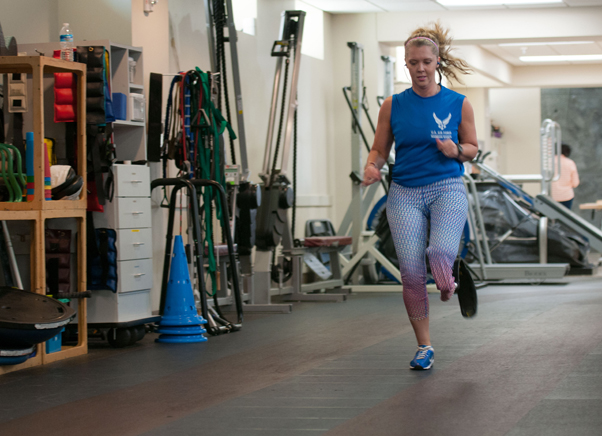BETHESDA, Md. (AFNS) — After a sprint around an indoor track with her prosthetic running blade, Heather Carter stopped, visibly tired. She smiled and began to sprint another lap.
The medically retired senior airman once rounded the bases for the Air Force softball team until a freak accident severely injured her left leg as she raced to first base during a game in 2010. Four years and many surgeries later, she chose to have the leg amputated.
“I figured if you’re going to do something, you may as well go all out,” she said, jokingly.
Through therapy at Walter Reed National Military Medical Center, she’s learning how to run again with a prosthetic for a chance to return to competitive softball — this time with the Wounded Warrior Amputee Softball Team, which travels the nation to play against able-bodied teams.
In early June, Carter, 30, was able to practice batting in the team’s exhibition game in Grand Forks, North Dakota.
“It was the first time that I hit the field since the injury,” the Barrington, Rhode Island, native said. “I was extremely nervous and my legs were shaking, but it was so great to be on the field.”
Goal oriented
Physical and occupational therapists at Walter Reed’s Military Advanced Training Center offer specialized care to Carter and other amputees to help them reach their goals.
Following an amputation, either by choice or from a traumatic injury, therapists work to strengthen a patient’s residual limb before they’re fitted for a prosthetic and learn to walk with it. The entire process can last anywhere from a few months to a few years, depending on the extent of the injuries.
“After that, the sky’s the limit to whatever their goals are,” said Army Capt. Nicole Brown, one of the center’s physical therapists.
The center uses a sports medicine model that also improves a patient’s balance and endurance, while introducing them to various activities, from reintegration trips in public places to adaptive sports. Some patients go on to play in Paralympic-style competitions like Invictus and Warrior Games.
“A lot of patients actually end up with more opportunities that they were never exposed to without coming here,” Brown said. “They realize that they still can do a lot of things, and, in some situations, even more than they were doing before their injuries.”
Road to recovery
Being realistic along their emotional roads to recovery is key for patients, who are missing one or even all four limbs, along with other devastating injuries. They may never have the same body as before, but they can still get their lives back.
“We’re giving them the opportunity to be the best versions of themselves,” Brown said. “That could be back to doing what they were doing before being injured or learning new things.”
Senior Airman Kyle Cook, who lost his right leg in a motorcycle crash in September, said he hopes to return to his weightlifting routine after he trains with his prosthetic leg.
“I’ll be able to walk to and from the gym and do what I used to do,” the Franklin, Pennsylvania, native said.
Cook, 22, expects it will take up to a year to be fully functional with a prosthetic. During that time, he’ll also strengthen his left leg, which suffered broken bones, nerve damage and torn knee ligaments in the crash.
“I didn’t have much function in my left leg at all,” he said, adding that he can now bend his knee. “It’s a slow recovery to getting my strength back. It’s just going to take time.”
To fulfill his goal of hitting the weights again, he tries not to think about his current limitations.
“In every kind of negative situation, there’s always going to be a positive,” he said. “For me, that’s just being able to walk. You take that for granted, but now I don’t.”
Custom fit
Prosthetics are tailored to every patient, with many modifications done in-house, to help them walk or perform another physical activity. Patients are consulted to ensure they get a comfortable, snug fit with the lightweight device weighing less than the actual limb lost.
“Each individual is totally different on their fit of their prosthesis and how they use it,” said David Beachler, a prosthetist at Walter Reed. “If they’re not fit properly in the socket, they’re not going to wear it.”
High-tech prosthetics are also available, such as intuitive prosthetic systems that hone in on pattern recognition for patients with upper-limb amputations. The devices provide more control and a quicker response when using a prosthetic hand.
“You just think about firing those muscles to open or close the hand,” Beachler said.
Activity-specific prosthetics, whether for rock climbing, running, fishing or even snowboarding, are offered to amputees so they can enjoy being outdoors and build the confidence therapists look to instill in them.
“We try to get them back to some sense of freedom and independence in their activities,” said Bob Bahr, a physical therapist.
Bahr, who has worked at Walter Reed for 17 years, has helped Carter train on her running blade. To him, the joy of seeing a lower-limb amputee standing, especially for the first time, makes his efforts worthwhile.
“To watch them stand and walk on the parallel bars can be a very emotional event,” he said. “It’s the first step to them getting back to having some sense of normalcy again.”
Running the bases on a softball field would be Carter’s idea of normalcy. She knows that the biggest obstacle standing in her way is a negative attitude.
“A lot of it is your own fight and determination to not give up,” she said.
“When you stop trying, you stop accomplishing.”
All the pain and fatigue endured in therapy sessions will hopefully pay off when she does compete in a real game and overcomes the trauma that was dealt to her.
“Just to be able to get back out there, it would make me feel that I didn’t lose the last six years of my life,” she said.