Senior Defense Department health officials detailed what the department is doing to support the whole-of-government assault on the coronavirus pandemic.
Army Lt. Gen. (Dr.) Ronald J. Place, director of the Defense Health Agency, and Navy Surgeon General Rear Adm. (Dr.) Bruce L. Gillingham told Pentagon reporters March 19 that the military medical establishment is looking at all ways to support Americans.
The Defense Health Agency has had a crisis action team in place for a while, Place said, looking at patient concerns and patient care, as well as equipment, blood supply monitoring and sharing DOD capabilities. “We’re looking at issues that become familiar to you by now — bed space, military health capabilities and capacity, the trade-offs of shifting resources from one need to another, assisting people with self screening, triage and testing of patients,” he said.
The general noted that daily call volume to the Military Health System nurse advice line has jumped 500% to at least 8,000 calls, and sometimes in excess of 10,000 calls per day.
Changes will happen in the health system as a result of COVID-19, the DHA director said. “Within our system, we’re evaluating reducing elective procedures to increase capacity,” Place said. “I’ve directed doctors and nurses and staff physicians to shift responsibilities for clinical patient care as much as possible. We’re looking at how our clinics and hospitals might be able to surge bed space that isn’t currently being used for patient care. The list goes on.”

One example of this is the mobilization of the hospital ships USNS Comfort and USNS Mercy to aid stricken communities. The Comfort — based in Virginia — will sail to New York. The Mercy will sail from San Diego next week to a port to be determined, Gillingham said. Each ship has a 1,000-bed capacity.
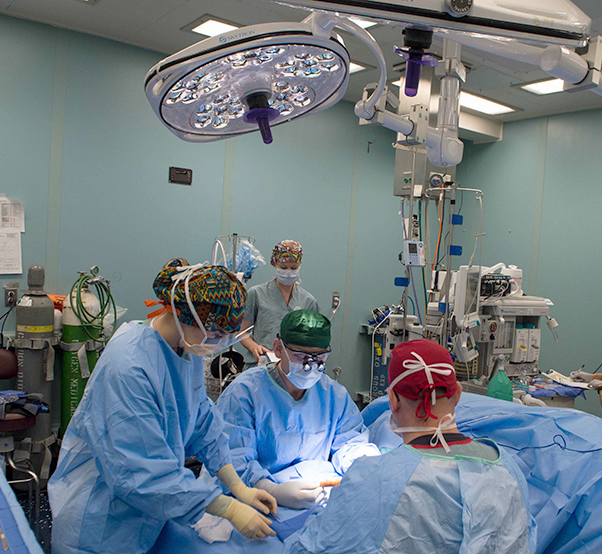
As to be expected, the ships’ medical crews are world-class trauma specialists, and that is what they will do when deployed, Gillingham said. People will still have car accidents, and there will still be shootings and other forms of trauma. Those patients will be treated aboard the ships, leaving the local hospitals to concentrate their scarce resources on COVID-19 patients, he explained.
“The preparations for the ships and the crews to run them fall under Fleet Forces Command,” he said. “But as the Navy surgeon general, I’m responsible for putting together the medical teams that will staff the ships and run the medical facilities aboard.”
He said the core members of the medical staffs are reporting today to ready those ships for their missions. “We can adjust the staffing as we go as we get a better sense from the local leadership of what they need,” he said.
Gillingham is working with the Defense Health Agency to get medical staff, so the doctors, nurses and support staff will come from all services. But with those staff members leaving military medical facilities, the mission of caring for the 9.5 million beneficiaries of the Defense Health Agency must continue, he said, and officials will keep an eye on the care for the communities they serve.